Hormonal hair loss, clinically known as androgenetic alopecia, is a prevalent condition impacting both men and women. It is characterized by progressive thinning of hair due to hormonal influences, particularly androgens such as dihydrotestosterone (DHT). dermatologist for hair loss and treating scalp and hair disorders are essential in evaluating, managing, and mitigating the effects of hormonal hair loss using a clinical and evidence-based approach.
Hormonal hair loss results from a complex interplay of genetics, endocrine function, and age-related changes. In males, this often appears as a receding hairline and vertex balding, while in females, diffuse thinning over the crown is more typical. The condition is chronic and progressive, making early diagnosis and continuous management important for maintaining hair density and follicular health.
The initial step in managing hormonal hair loss involves a comprehensive evaluation. Dermatologists begin with a detailed medical and family history, followed by a clinical scalp examination. Tools such as trichoscopy allow for magnified visualization of hair shafts and follicular units, revealing hallmark features of androgenetic alopecia, such as hair diameter diversity and follicular miniaturization.
In some cases, dermatologists may request laboratory investigations to rule out contributing factors or coexisting conditions. Common tests include serum ferritin, thyroid function panels, and hormone profiles, particularly in women presenting with signs of hormonal imbalance such as irregular menstruation or acne.
Once a diagnosis is confirmed, treatment planning is individualized. Dermatologists select therapies based on clinical evidence, patient age, severity of hair loss, and comorbidities. Topical therapies remain foundational. For example, solutions containing minoxidil have been demonstrated in peer-reviewed studies to promote hair regrowth and reduce shedding by extending the anagen (growth) phase of hair follicles.
In cases where hormonal influence is pronounced, oral therapies may be introduced. Anti-androgen medications, such as 5-alpha reductase inhibitors, work by reducing the conversion of testosterone to DHT, thereby slowing follicular miniaturization. These are generally more common in male patients; however, some women may benefit from hormone-modulating treatments under close medical supervision.
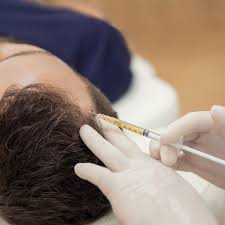
Adjunct therapies, such as platelet-rich plasma (PRP) injections and microneedling, are also used in some dermatology practices. These techniques aim to stimulate follicular activity and support hair density, particularly when used in combination with pharmacologic treatments.
Patient education is a central part of dermatologic care. Individuals are advised that hormonal hair loss is usually a long-term condition that requires consistent treatment for sustained results. Dermatologists provide guidance on realistic outcomes and offer long-term monitoring to track progress and make necessary adjustments.
In Fort Worth and other clinical settings, dermatologists contribute significantly to community health by addressing hair loss with a scientific and compassionate approach. Their role extends beyond cosmetic concerns, as they support physical and psychological well-being through individualized medical care. By promoting access to accurate diagnoses and evidence-based treatment, dermatologists help improve hair health outcomes for patients across all communities.